Pain is the most usual factor people look for care, yet it is commonly the least constantly handled. A certificate course hurting monitoring can close that space, converting guidelines into reliable bedside practice. The toughest programs couple clinical roughness with the genuine restrictions of rescues, wards, centers, and rehab fitness centers. If you operate in acute care, primary care, paramedicine, nursing, physical rehabilitation, or allied wellness, constructing competence in both evaluation and treatment modifications end results swiftly. I have seen it in my own technique: fewer readmissions, much shorter lengths of stay, and patients who lastly sleep through the night.
This guide goes through what a thoughtful pain administration certification resembles, how to pick a course that fits your setup and range, and a useful path to succeed once you enlist. Along the way, I'll touch on specialized choices like puaeme008 give pain management for emergency situation -responders, pain monitoring programs for nurses and physio therapists, and short programs in pain administration that slot right into active rosters.
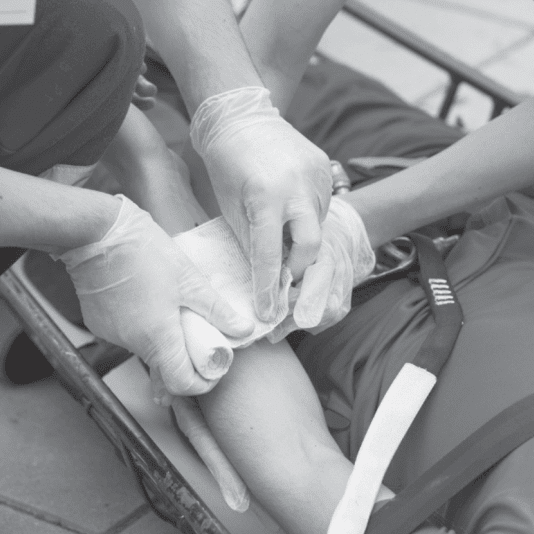
Why discomfort management training is worth your time
Pain is not just a sign, it is a chauffeur of problems. Unchecked sharp pain elevates catecholamines and can intensify heart ischemia, hinder ventilation, and slow mobilization. Improperly taken care of persistent pain usually spirals right into deconditioning, state of mind conditions, and polypharmacy. When medical professionals complete a pain administration program that highlights assessment precision, multimodal treatment, and interaction, the effect is measurable. On a surgical device where we executed standard discomfort evaluations and day-to-day analgesic optimization, the ordinary time to initial mobilization visited approximately a third over one quarter. Patient fulfillment ratings increased, however much more notably, post-op lung problems fell.
A certification signals to your group that you can structure care with intent, not behavior. It also helps in credentialing and advanced duties. Lots of organizations currently acknowledge a discomfort administration certification as proof of continuing competence, especially for increased practice registered nurses, medical nurse specialists, and extended-scope physiotherapists.
What a solid certificate training course hurting monitoring covers
The finest pain monitoring training courses avoid the catch of being a pharmacology lecture stitched to a set of pain scales. They develop a useful structure you can use on a disorderly shift, throughout a silent ward round, or in a long consult with a complex client. A total program normally includes:
Foundations of pain physiology and the lived experience. Anticipate protection of nociceptive versus neuropathic discomfort, outer and central sensitization, and just how concern, rest, and previous trauma reshape pain processing. Great instructors attach theory to vignettes you'll actually identify, like the post-herpetic neuralgia patient that enhances only after you deal with allodynia and sleep separately.
Assessment with subtlety. Discomfort ratings are the starting point, not the destination. You must exercise useful objectives, movement-based assessment, and risk stratification for opioid-related damage. Pediatric, senior citizen, and cognitively impaired evaluations need to be greater than a sidebar.
Pharmacological strategies across setups. Short-acting versus long-acting opioids, opioid-sparing routines, neuropathic representatives, ketamine for specific indicators, and local anesthesia fundamentals. Look for product on risk-free deprescribing, kidney and hepatic application, and pharmacogenomic factors to consider where relevant.
Nonpharmacological and corrective techniques. Warmth, cool, TENS, pacing, rated exposure, mindfulness, and sleep health issue if they are supplied with framework and follow-up. Physio therapists must see graded motor images and desensitization techniques in action, not simply on slides.
Communication that moves results. Pain is a negotiation, framed by trust fund. Programs should educate scripting that confirms pain while setting useful targets, plus brief treatments for catastrophizing and kinesiophobia.
Safety, equity, and systems. Naloxone co-prescribing, PDMP use where suitable, taking care of opioid use condition without stigma, social safety and security, and access barriers for rural and remote clients. For healthcare facilities, include acute pain service rise requirements and handover standards.
Documentation and metrics. If you can not determine your impact, you can not sustain it. Good programs show you just how to build problem listings tied to pain medical diagnoses, track feature, and make use of high quality indicators that endure an audit.
Mapping the training course to your role
You do not require every component at the same depth. Match the program to your day-to-day decisions.
Nurses in acute treatment gain from tight assessment, PRN optimization, safe titration methods, and nonpharmacological methods they can provide at the bedside. Discomfort administration training for nurses need to include step-by-step analgesia assistance, delirium and discomfort distinction, and escalation formulas straightened with the facility.
Physiotherapists need durably applied movement-based approaches. Discomfort monitoring programs for physio therapists must drill rated direct exposure, load progression, are afraid evasion therapy, and ways to incorporate analgesic timing with treatment sessions. In post-surgical rehabilitation, recognizing when to request a nerve block testimonial can conserve days.
Primary care medical professionals and pharmacologists need persistent discomfort frameworks. This includes taper plans, rest normalization, perioperative opioid administration, and interprofessional recommendation criteria for pain facilities, psychology, and interventional specialties.
Paramedics and very first -responders function under time pressure. Systems like puaeme008 provide pain monitoring, usually referred to as puaeme008 supply discomfort management within professional training bundles, concentrate on prompt assessment, secure management of analgesics in the field, nonpharmacological methods throughout extrication, and handover that preserves analgesic momentum. If you run in this atmosphere, choose a program straightened with your territory's formulary and professional technique guidelines.
Anatomy of a practical learning pathway
A certificate training course hurting management typically runs in combined format. Expect self-paced discovering components integrated with workshops or substitute cases. Programs range from short training courses hurting administration that take 6 to 12 hours, to even more extensive pain administration qualification training courses that run 40 to 80 hours with analyses and situation logs.
I urge candidates to structure their research study around 3 arcs: assessment mastery, treatment fluency, and interaction under restraint. The web content could look similar across programs, yet sequencing matters. Technique evaluation scripts with coworkers early, not after pharmacology. Learn to ask, then to act, then to review.
Clinical exposure, also if substitute, does the hefty lifting. I have seen learners boost most after they present two or three longitudinal cases. One was a 58-year-old with failed back surgical treatment disorder, averaging 4 hours of rest and walking much less than a block. After setting a two-week useful target, coordinating a neuropathic agent titration, and changing therapy timing, his six-minute stroll improved by 60 meters and he cut evening awakenings in fifty percent. The numbers were simple, the strategy was systematic, and the modification stuck.
Emergency discomfort monitoring deserves its own lane
Acute discomfort in the area and in emergency divisions has different dangers and chances. You commonly do not recognize the standard opioid direct exposure, comorbidities, or background important usage, yet delays substance suffering and issues. A focused emergency situation pain management module stresses:
Rapid differential diagnosis of discomfort types on thin info. That includes identifying time-critical conditions where analgesia need to not wait, yet the option of representative and path matters to avoid masking peritoneal signs or neurologic deficits.
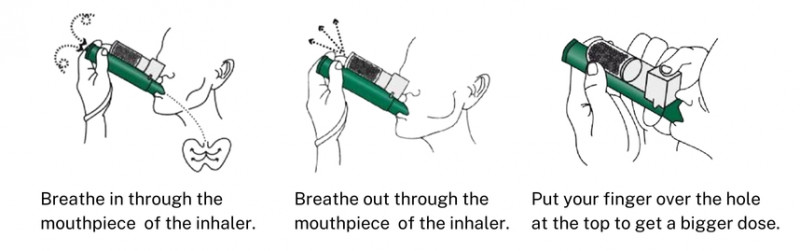
Analgesic pharmacology tailored to prehospital and ED methods. Inhaled analgesia, intranasal alternatives, IV titration with safety and security checks, and pediatric application that is easy to compute quickly. Ketamine calls for clear indicators and contraindications.
Nonpharmacological strategies that get time and boost outcomes. Splinting done appropriately, cold application, positioning for dyspnea and pleuritic discomfort, and training breathing for extreme anxiety and panic where pain intensifies distress.
Handover technique. If you provide significant analgesia in the area, handover should consist of timing, effect, and risk flags to prevent rebound discomfort or double dosing. Programs constructed around puaeme008 offer pain monitoring highlight this handover stringently.
I have viewed new paramedics, when trained and monitored through a loads calls, slash time-to-analgesia by fifty percent without a solitary safety and security incident. The difference was confidence anchored to procedure, not bravado.
Choosing among pain monitoring training courses without getting lost
Marketing language looks similar across service providers. Sort programs by that designed them, exactly how they evaluate you, and whether the content lines up with your range of technique. Integrity shows up in little details, like application modifications for renal disability or case studies that consist of consent for nerve blocks.
You also wish to see a plan for continuous competence. Some programs supply a pain management certification training course with a single analysis, then recommend annual refreshers. Others construct in reflective method and situation audits. If you prepare to maintain a pain administration certification that strengthens your resume, pick the latter. It will make your profile more powerful and your technique safer.

Costs differ extensively. Short training courses may be inexpensive and focused, a good suitable for brand-new graduates or teams attempting to level up a single ability like neuropathic discomfort. Comprehensive pain management training courses typically validate greater charges with faculty access, supervised method, and identified certification. Verify what you get: downloadable devices, exam efforts, proctored OSCEs, and assistance for office projects.
The detailed path to certification and impact
Here is a portable, useful advanced pain management for physiotherapists sequence that has benefited several clinicians I have mentored. It keeps momentum high and concentrates on modifications that stick.
- Clarify your range and setting. Note the three most common discomfort scenarios you manage weekly, and one high-risk circumstance you fear. This shapes your training course selection and study plan. Pick a course that matches your territory and role. If you remain in prehospital treatment, a program straightened with puaeme008 supply discomfort monitoring or your neighborhood equal conserves translation work. Registered nurses ought to seek pain administration training for nurses with facility-specific escalation pathways. Physiotherapists must make certain there is considerable material on graded direct exposure, pacing, and discomfort education. Front-load evaluation abilities. In the very first two weeks, manuscript your history-taking, functional goals, and risk stratification. Practice on 2 people and one colleague. Record times and outcomes. Implement one modification each week. Week one, readjust PRN timing and nonpharmacological assistances. Week two, introduce or enhance a neuropathic representative if indicated. Week three, change treatment sessions around analgesic heights. Constantly track function. Build a little dashboard. Track numerical discomfort ratings just as context. Focus on feature: distance strolled, rest hours, time to set in motion, or return to function steps. Evaluation once a week and show your mentor or team.
This is the very first of the two listings in this write-up, purposefully brief. Each item opens the next, and the last control panel both confirms expertise and encourages cynical colleagues.
Integrating pain administration right into team workflows
A certificate changes your method, however the bigger win is team consistency. Pain administration training courses that call for a job element typically ask you to apply a tiny workflow renovation. The most effective prospects select something visible and reversible, like a daily short courses in pain management analgesia optimization huddle on a post-op ward, or a pre-physio analgesic timing procedure in rehabilitation. Success depends on:
Leadership that values little victories. Beginning with a two-week pilot, then increase. If your pilot shortens the early morning mobilization window by 15 mins across 4 individuals, your unit has hours of performance obtained weekly.
Clear possession. A single person updates the pain board, one more activates rise if targets are missed for two days, and a third audits managed compound settlement. When nobody has pain, discomfort has the shift.
Data that informs a human story. A graph revealing rest hours and night-time pain together with quotes from the person is influential. I have never seen a doctor ignore sleep restored after 2 evenings of targeted adjustment.
Workflows ought to also acknowledge edge cases. Individuals with chronic opioid therapy requirement different procedures. Those with unmanaged PTSD or high degrees of catastrophizing demand very early psychology referral. Not every device has these services in-house, so a well-constructed pain monitoring accreditation program need to aid you build recommendation paths and scripts for scarce resources.
The pharmacology you will actually use
A solid program equilibriums detail with energy. You ought to leave able to do the complying with without reaching for a recommendation every single time:
Dose non-opioids actively. Paracetamol and NSAIDs still carry the opioid-sparing load, but just if you make use of appropriate timetables and account for kidney, hepatic, and bleeding threats. Lots of new graduates underdose out of care that is unnecessary with proper screens.
Recognize when to pick an opioid, which one, and exactly how to taper. Oxycodone, morphine, hydromorphone, and fentanyl each have particular niche advantages relying on organ function and route accessibility. Prevent incorporating long-acting and short-acting opioids without a clear strategy. Support treatment to practical objectives and daily review.
Introduce neuropathic representatives with timelines that match reality. Gabapentinoids and SNRIs require days to weeks to reveal result. Programs must stress titration schedules, autumn and sedation threats in older adults, and techniques for discontinuation when they fail to help.
Understand procedural and interventional choices sufficient to refer suitably. Area blocks and regional anesthetic can be transformative post-op, however timing and client option matter. Physiotherapists, particularly, take advantage of understanding when to ask for a block testimonial to open very early mobilization.
Use ketamine carefully. Sub-dissociative dosing can be reliable for certain acute pain circumstances, yet needs clear protocols and surveillance. Excellent training programs instruct both prospective advantages and the behavioral side effects that agitate people and staff when unanticipated.
The goal is not universal recall, it is risk-free and definitive activity when your individual is in front of you.
Communication and assumption setting
Pain management is half pharmacology, half discussion. You will discover to claim things that change a person from a numerical target to a useful one. Instead of appealing absolutely no pain, you could use consistent gains: stroll to the mail box, after that around the block, then to the park. This reframing decreases distress and reduces the chase for intensifying dosages that dissatisfy everyone.
For family members, manuscripts help when discomfort lingers despite best shots. Clarify the strategy, adverse effects to watch for, and what improvement will certainly resemble each day. In one clinical ward, offering a one-page pain plan that included convenience actions households could aid with cut call bell usage over night and improved mood on both sides of the bed.
Cultural safety rests inside interaction. Pain expression varies throughout cultures and people. Training should show you to ask open questions, avoid presumptions about stoicism or overestimation, and engage interpreters early when language barriers exist.
Assessment risks and just how great training courses instruct you to prevent them
I have seen 2 common mistakes in clinicians prior to extra training. Initially, overreliance on a single numeric rating. Second, failing to reassess. A pain score without context can mislead, specifically in older adults with ecstasy or in patients that underreport to prevent being identified. The repair is easy and teachable: set ball game with a functional objective and a concentrated test, then reassess at predictable intervals after an intervention. Lots of certificate programs require you to submit two review notes per case, a behavior that sticks.
Another mistake is the one-size-fits-all analgesic. If your default is a single opioid, you will certainly overuse it. Multimodal programs that respect renal function and procedural context are much safer and usually more reliable. An organized pain management course should provide counterexamples that test reflexes and provide a much better algorithm.
Assessment, certification, and maintaining competence
Pain management certification commonly consists of on-line tests, case-based short answers, and, in the stronger offerings, observed structured medical exams. I learned most from OSCE terminals that required me to work out goals with a standard person while explaining risks of opioids and setting a clear plan for the following 48 hours. If your program uses optional OSCEs, take them.
After you make a discomfort administration certification, prepare for refresher courses. Medication formularies transform, therefore do standards for opioid use, naloxone distribution, and perioperative care. The most defensible method is to complete a brief update every 12 to 24 months. If your technique consists of emergency situation care, look for components aligned with upgraded medical technique standards comparable to those embedded in puaeme008 offer discomfort management.
Keep a little portfolio: a log of tough instances, your audit results on feature metrics, and reflections on a minimum of 2 situations where your plan changed mid-course. This is what turns a credential into an expert asset.
Special tracks for nurses and physiotherapists
Pain management training for nurses should concentrate on 3 layers: exact assessment, protocol-driven titration, and nonpharmacological supports registered nurses can supply right away. Programs that include simulation for tough discussions work well, specifically for tapering demands or managing household assumptions. Registered nurses often become the champs of daily analgesia optimization, which is where the most significant gains hide.
Pain monitoring training courses for physiotherapists must push beyond education into graded exposure that is measurable. I have seen specialists transform a client's expectation with a six-week plan that stabilizes load and worry. Programs that need specialists to send pre and post practical metrics elevate the requirement. When therapists and registered nurses straighten, the morning home window, about one hour after analgesia, becomes a reliable platform for progress.
Short programs versus detailed certification
Short training courses suffering management have their location. For groups needing a fast tune-up or to standardize a single method change, a focused 6 to 8 hour course is warranted. Utilize them to improve pediatric application security, to present a new nonpharmacological toolkit, or to tackle neuropathic pain options.
A full pain management qualification course is better if you intend to be a best source or to lead top quality improvement. These programs give you breadth, supervised technique, and an assessment that stands in efficiency reviews. In numerous systems, such a certificate supports applications for innovative placements or profile pathways.
A small readiness checklist prior to you enroll
- Define your end result: promo, function growth, or far better individual circulation on your unit. Confirm alignment: does the training course match your drugs, methods, and referral networks? Secure time: block secured slots for study and 2 professional situations to use learning. Arrange mentorship: a teacher or elderly clinician who will examine your cases. Plan your audit: choose one useful statistics you will track for four weeks post-certification.
This second and last listing maintains you truthful. When medical professionals total these actions, they are much more likely to apply adjustment as opposed to take in content and wander back to old habits.
What success looks like six weeks after certification
Gauge success on the ground, not in the framework on your wall. On a surgical floor, expect earlier mobilization, fewer nighttime calls for advancement discomfort, and much shorter lengths of stay in uncomplicated instances. In primary care, search for less very early refill demands, even more regular useful gains, and better rest reported at follow-up. In prehospital treatment, monitor time-to-analgesia, damaging occasions, and handover top quality notes.
I collaborated with a local group that combined a certification training course with a solitary process change: a day-to-day evaluation of clients whose rest was interrupted by pain. Evening nurses applied a standard nonpharmacological method and rose targeted modifications in the early morning. Within a month, the device reduced wakeful nights associated with pain by roughly a quarter, and daytime treatment sessions ran closer to schedule. None of this called for brand-new medicines. It required a shared language and a plan.
Final ideas from the center floor
Pain will certainly always be a moving target, shaped by biology, psychology, and context. A discomfort management certification gives you extra arrows in the quiver and the judgment to select the best one under pressure. If your course points to emergency discomfort monitoring, straighten your training with certified systems like puaeme008 provide discomfort monitoring. If you lead on a ward or in a facility, think about a comprehensive pain administration certification that consists of quality renovation and case supervision. Nurses and physio therapists will certainly discover committed programs that sharpen the tools they make use of daily.
The genuine mark of success is not the certification itself, however a client that informs you they can lastly clothe without assistance, stroll their dog, or rest without worry of the evening. That is what this training is for, and it is accessible when coursework translates into consistent practice.